[ad_1]
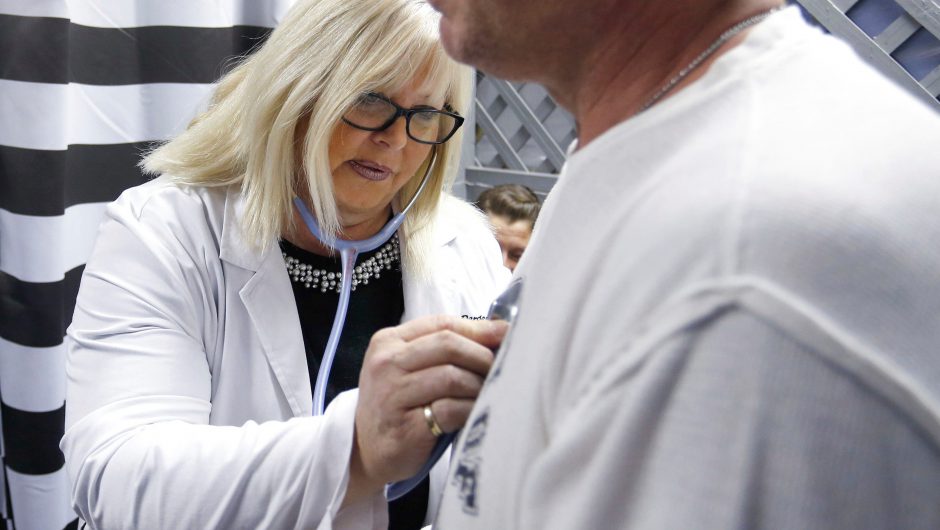
A nurse rests in a makeshift ward at an emergency Covid-19 care centre in New Delhi, India – T. Narayan/Bloomberg
It had taken a long time for Pramila Minz, 28, to persuade her mother to relocate from her remote village deep in Odisha’s tribal belt to New Delhi. After her mother, Gurubari Minz, 55, began showing coronavirus symptoms and had a suspected stroke, Ms Minz was secure in the belief her mother would receive the best possible healthcare now she lived in the capital.
She took Mrs Minz to Safdarjung Hospital late on the evening of June 10. To her horror, after conducting a CT scan and X-ray, a doctor refused to admit her because of a shortage of staff and beds.
Mrs Minz was rejected by five other major hospitals in New Delhi during a frantic 24-hour search.
Her condition was worsening by the minute. She was experiencing increasing breathing difficulties and drifting in and out of consciousness. Despite these grave symptoms, her daughter still could not get her mother admitted, despite explaining to doctors that she had suffered a stroke 18 months previously and therefore had comorbidities, making her extremely vulnerable to coronavirus.
Social media is full of similar stories, helping to build a picture of a healthcare system in crisis as India battles the fourth-highest number of cases globally.
The extreme challenges faced by hospitals have been exacerbated by the number of doctors and nurses contracting coronavirus themselves. Dr Ramanan Laxminarayan, director of the Centre for Disease Dynamics, Economics and Policy, says: “Everyone is focused on beds and ventilators but I am more concerned about the shortage of medical personnel.
“Qualified doctors and nurses are working flat out and are exhausted. They then face additional stigma in their communities.
A vendor sells tomatoes at Azadpur wholesale vegetable market after the government eased a nationwide lockdown – XAVIER GALIANA / AFP
“Unless there is a national effort to organise and leverage all available medical expertise in the country, it is going to be a long Covid season in India”.
Pre-coronavirus, Indian public hospitals were already severely understaffed, with a nationwide shortage of 600,000 doctors and two million nurses. This scarcity is compounded by the high proportion of quack doctors among the 1.2 million registered – over half of doctors have no medical qualifications, according to the World Health Organisation.
Story continues
For years, the Indian government failed to allocate more funding to train medical professionals to fill the staffing gap or provide existing healthcare professionals with the knowledge to provide advanced care. “Healthcare workers have been referred to as corona warriors,” says Dr Saurabh Sacchar at Safdarjung Hospital. “It can take 10 years and discipline to reach that stage – to develop a person who can work well independently in an intensive care unit, can work in a team, and decide what’s best for the patient.”
India’s public healthcare system is one of the most underfunded and outdated in the world, with less than £12 spent per person annually. Poor working conditions and a failure to increase wages have also prompted 100,000 doctors to emigrate to countries such as the UK and Australia.
Ms Minz saw for herself the shoddy conditions in many hospitals when she took her ailing mother around New Delhi, trying desperately to get her a bed. At one, there were not enough staff to lift her mother onto a stretcher and she had to do it herself.
A volunteer walks past disposable beds made out of cardboard at the campus of Radha Soami Satsang Beas, a spiritual organization, where a coronavirus care centre has been constructed in New Delhi – REUTERS/Danish Siddiqui
Ms Minz is haunted by guilt for persuading her mother to move to the capital. “At one hospital, the doctors made me run around the wards,” she said. Eventually, Mrs Minz was admitted to Lok Nayak Jai Prakash Narayan Hospital after Ms Minz’s local MP intervened following a plea on social media.
This week, India registered 500,000 coronavirus cases but its peak is not predicted until November, with the virus set to spread rapidly in the country’s densely-populated cities. New Delhi has the largest number of infections out of any city in India at 73,780 but the city’s Deputy Chief Minister has predicted that by the end of July, it will see 550,000 infections and require 80,000 more hospital beds.
“Our current healthcare workforce is under a lot of pressure at this moment not only due to the duration of the epidemic until now but also to cope with the spurt in cases. We wonder how the government will manage to get enough healthcare workers to support the expansion of hospitalisation facilities,” said Malini Aisola, co-convenor of the All India Drug Action Network.
The shortage of healthcare professionals is being exacerbated by the failure of the Indian Government to provide adequate personal protective equipment, with doctors contracting coronavirus from the patients they are treating.
Healthcare professionals in Delhi, Mumbai and Kolkata told the Daily Telegraph that while supplies had increased since the lifting of a nationwide lockdown on June 1, there were still shortages and they were often having to re-use torn PPE.
“We understand these are difficult times, and it would be extremely wrong to think of our selfish interest now,” said a nurse at one Delhi hospital, on condition of anonymity. “We are not asking for money or anything like that. After all that we try to do, we just want to be treated like humans.”
Another nurse in New Delhi said over 300 members of staff in his hospital had tested positive for Covid-19, and blamed a lack of protection. “The shortage of staff is there at every level, from doctors and nurses to housekeeping,” he said, also on condition of anonymity. “This is the main issue we are facing now.”
A government doctor in a hospital in the city of Surat told the Telegraph that shortages meant each employee was having to care for 30 coronavirus patients.
A health worker in personal protective equipment collects a sample using a swab from a person at a local health centre – REUTERS/Adnan Abidi
Private hospitals are not faring well either, with three facilities in Mumbai closing after a large number of staff tested positive for coronavirus. Healthcare professionals are facing increasing stigma and pressure from their families to stop coming to work.
“Most of the staff left the hospital when it was converted to treat Covid-19 patients, because their families said they shouldn’t be around the sick,” said Dr Solanki, owner of the Dharamveer Solanki Multispeciality Hospital in New Delhi, which specifically treats coronavirus patients. “We have had to hire new nursing, laundry and security staff four or five times over the last 20 days, because everyone is so scared, they refuse to come”.
Dr Solanki fears he will have to shut his hospital down and that many others will follow suit over the next few months, due to staff shortages.
Reports of patients such as Mrs Minz being refused admission by hospitals prompted the Indian government to step in and take control away from the government of Delhi. It first proposed the institutional quarantining of every positive case but this was overturned after the authorities in Delhi said they had nowhere near enough healthcare staff to cope with the sudden influx.
To cope with the predicted 80,000 extra beds it will need by July 31, the Delhi government is converting 500 train carriages and setting-up a 10,000-bed Covid-19 care facility in an ashram in the centre of the city. Eyebrows were raised when it announced 25 luxury hotels would house patients, with unqualified staff expected to deliver medicines instead of room service.
Relatives of a coronavirus victim wear protective gear at the funeral – REUTERS/Adnan Abidi
The upcoming couple of months will be “mayhem”, predicts public health expert, Dr Yogesh Jain. The German Embassy in New Delhi warned its citizens this week that they face “little or no chance” of any hospital admission.
The onset of India’s annual monsoon, and with it a surge in diseases such as malaria and dengue fever, will see a further spike in patients needing hospitalisation.
There is, however, good news for Mrs Minz, who has been moved from an ICU to a general ward after 17 days. Ms Minz hasn’t received a phone call from anyone caring for her mother since her admission and has instead been receiving updates from a sympathetic ambulance driver she befriended at the hospital. She has been told that while her mother is showing signs of recovery, her prolonged battle against coronavirus is a result of her delayed admission.
“I will do all that it takes to have her back. Will you please pray for us?” she asked.
[ad_2]
Source link